Table of Contents
- Key Points
- What Is An Actinic Keratosis?
- What Does An Actinic Keratosis Look Like?
- The Connection Between An Actinic Keratosis and Skin Cancer
- Actinic Keratoses Treatment Options
- Prevention: Your Best Defense
- Take Control of Your Skin Health Today
- References
Key Points
- Actinic keratoses, which affect upwards of 1/5 of all Americans, appear as rough, scaly patches on sun-exposed skin.
- They can progress to squamous cell carcinoma or other types of cancer, if left untreated, making early detection and treatment essential.
- Understanding the basics of actinic keratoses, including available treatment options, can be life-saving for anyone affected.
If you have ever noticed rough, scaly patches on your skin that will not go away, you’re not alone. More than 58 million Americans are currently living with an actinic keratosis (AK), making it one of the most common skin conditions treated by dermatologists.1
While these crusty spots may seem harmless at first glance, they represent something more serious: a warning sign that your skin has sustained significant sun damage and that skin cancer could be on the horizon.
At Rogers Dermatology, we believe that education is your first line of defense against skin cancer. Understanding actinic keratoses—what they look like, why they matter, and how we treat them—can help you take proactive steps to protect your skin health for years to come.
What Is An Actinic Keratosis?
An Actinic keratosis, also called “solar keratosis,” is a precancerous skin growth that develops after years of sun exposure. These lesions appear as rough, scaly patches on sun-exposed areas of the body. While they start as benign growths, they have the potential to transform into squamous cell carcinoma, one of the most common types of skin cancer.2
The word “actinic” refers to ultraviolet radiation from the sun, which is the primary cause of these lesions. Over time, UV rays damage the DNA in your skin cells, causing abnormal cell growth that manifests as AK.3
In a way, you can think of an actinic keratosis as your skin’s way of raising a red flag. It is telling you that damage has occurred and that continued neglect could lead to more serious consequences.
What Does An Actinic Keratosis Look Like?
Recognizing actinic keratoses early is crucial for preventing progression to skin cancer. Here is what to look for:
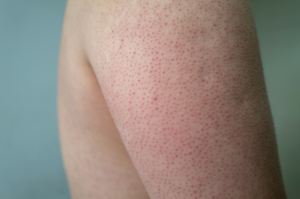
Appearance and Texture
- Rough, dry, or scaly patches that feel like sandpaper when you run your finger over them
- Flat to slightly raised lesions
- Crusty surface texture (similar to that of warts)
- Size ranging from a pinhead to larger than a quarter
- Color variations, including pink, red, brown, tan, or flesh-colored patches
Common Locations
- Face, especially the nose, forehead, and cheeks
- Ears
- Scalp (particularly in people with thinning hair or baldness)
- Neck and décolletage
- Backs of hands and forearms
- Lips (called “actinic cheilitis”)4
- Shoulders and upper back
One of the most distinctive features of an actinic keratosis is that it is often easier to feel than to see. Many patients first discover these lesions by touch—running their hand across their face or scalp and noticing an unusual rough spot that was not there before.
The Connection Between An Actinic Keratosis and Skin Cancer
Here is the critical information every patient needs to know: while not all actinic keratoses will become cancerous, they represent a significant risk factor for skin cancer development. Studies suggest that between 5 and 20 percent of untreated actinic keratoses will progress to squamous cell carcinoma within a decade.5
Understanding the types of skin cancer and their warning signs is essential for anyone dealing with an actinic keratosis:
- Squamous Cell Carcinoma: This is the most common type of skin cancer in the United States, and (as mentioned) is highly associated with AK. It can appear as a firm red nodule, a scaly patch with a crusted surface, or a sore that heals and reopens. Early detection and treatment are crucial.6
- Basal Cell Carcinoma: While not directly caused by AK, people with multiple actinic keratoses often develop basal cell carcinoma as well, since both conditions stem from cumulative sun exposure.7
The presence of an actinic keratosis is also a marker that your skin has sustained significant UV damage, which increases your overall risk for all types of skin cancer, including melanoma—the deadliest form.
Skin Cancer Symptoms and Warning Signs
Knowing what skin cancer looks like can save your life. 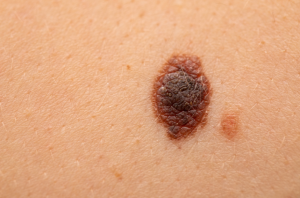 When examining your skin for signs of skin cancer, remember the “ABCDE rule” for melanoma and watch for these skin cancer symptoms:
When examining your skin for signs of skin cancer, remember the “ABCDE rule” for melanoma and watch for these skin cancer symptoms:
- Asymmetry: One half of the mole does not match the other half
- Border irregularity: Edges are ragged, notched, or blurred
- Color variation: Multiple colors or uneven distribution of color
- Diameter: Larger than a pencil eraser (6mm), though melanomas can be smaller
- Evolving: Any change in size, shape, color, elevation, or new symptoms like bleeding or itching
For non-melanoma skin cancers like squamous cell and basal cell carcinoma, watch for:
- Persistent sores that fail to heal within a few weeks
- Patches of skin that are red, scaly, and rough
- Shiny, pearly, or waxy bumps
- Flat, firm, pale, or yellow areas that resemble scars
- Bleeding or oozing from a skin lesion
If you notice any of these warning signs, schedule an appointment with a dermatologist in Greenville immediately. Early detection dramatically improves treatment outcomes for all types of skin cancer.
Actinic Keratoses Treatment Options
The good news is that treating an actinic keratosis is highly effective, especially when caught early. Rogers Dermatology offers multiple approaches, tailored to each patient’s unique needs.
Topical Medications
For patients with multiple lesions or those who prefer non-invasive options, prescription creams and gels can effectively eliminate actinic keratoses:
- 5-Fluorouracil (5-FU): Applied to affected areas for several weeks, this medication causes the abnormal cells to die off and be replaced by healthy skin.
- Imiquimod: This immune response modifier stimulates your body’s immune system to attack the precancerous cells.
- Diclofenac gel: A gentler option that works over a longer period, typically three months.
- Ingenol mebutate: A shorter treatment course, usually applied for two to three consecutive days.
In-Office Procedures
When topical treatments are not suitable or for isolated lesions, we offer several effective in-office procedures for actinic keratoses treatment:
- Cryotherapy (Freezing): The most common treatment method, liquid nitrogen is applied to freeze and destroy the abnormal cells.8 The treated area may blister and eventually peel away, revealing healthy skin underneath.
- Curettage: The lesion is scraped off using a specialized instrument called a curette. This may be combined with electrosurgery to remove any remaining abnormal cells.
- Chemical Peels: Medical-grade chemical peels can remove the damaged outer layers of skin, eliminating multiple actinic keratoses in treated areas.
- Photodynamic Therapy (PDT): A light-activated treatment where a photosensitizing agent is applied to the skin and then activated with specific wavelengths of light, destroying precancerous cells while minimizing damage to surrounding healthy tissue.
- Laser Therapy: Certain types of lasers can precisely target and remove actinic keratoses with minimal scarring.
Choosing the Right Treatment
During your consultation at our dermatologist office in Greenville, we will evaluate factors, including:
- The number and location of your actinic keratoses
- The thickness and severity of the lesions
- Your skin type and healing capacity
- Your lifestyle and treatment preferences
- Any previous treatments you have undergone
Our goal is to create a personalized actinic keratosis treatment plan that effectively eliminates your precancerous lesions while fitting seamlessly into your life.
Prevention: Your Best Defense
While treating an actinic keratosis is important, prevention is even better. Once you have developed AK, you are at a higher risk of developing more lesions and skin cancer. Here are essential steps to protect your skin:
- Use broad-spectrum sunscreen daily: Apply SPF 30 or higher every morning, even on cloudy days, and reapply every two hours when outdoors.
- Seek shade during peak UV hours: If possible, limit sun exposure between 10 a.m. and 4 p.m. when UV rays are strongest.
- Wear protective clothing: Long sleeves, wide-brimmed hats, and UV-blocking sunglasses provide crucial protection.
- Avoid tanning beds: Artificial UV radiation is just as damaging as natural sunlight.
- Schedule regular skin checks: Annual full-body skin examinations with a Greenville SC dermatologist can catch problems early.
- Perform monthly self-exams: Learn what is normal for your skin so you can spot changes quickly.
Take Control of Your Skin Health Today
Actinic keratoses may be common, but they should never be ignored. These precancerous lesions are a clear signal that your skin needs professional attention. The good news is that, with proper treatment and ongoing prevention strategies, you can dramatically reduce your risk of developing skin cancer.
Remember, your skin is your body’s largest organ, and it deserves expert care. Contact us today to schedule your consultation and take the first step toward healthier, safer skin. Because when it comes to an actinic keratosis and skin cancer, what you don’t know can hurt you, but what you do know can save your life.
References
- “Actinic Keratosis Overview,” Skin Cancer Foundation, November 2025, https://www.skincancer.org/skin-cancer-information/actinic-keratosis/.
- Mayo Clinic Staff, “Actinic keratosis,” Mayo Clinic, December 2022, https://www.mayoclinic.org/diseases-conditions/actinic-keratosis/symptoms-causes/syc-20354969.
- Lawrence Charles Parish, MD, “Actinic Damage,” International Academy of Cosmetic Dermagology, retrieved on December 1, 2025, from: https://iacdworld.org/actinic-damage/.
- “Actinic Cheilitis,” The Cleveland Clinic, May 2022, https://my.clevelandclinic.org/health/diseases/23007-actinic-cheilitis.
- Yoon-Seob Kim, Sun Shin, Seung-Hyun Jung, et al., “Genomic Progression of Precancerous Actinic Keratosis to Squamous Cell Carcinoma,” Journal of Investigative Dermatology, March 2022, https://www.sciencedirect.com/science/article/pii/S0022202X2102162X.
- “Squamous cell carcinoma,” University of Pennsylvania School of Medicine, retrieved on December 2, 2025, from: https://www.pennmedicine.org/conditions/squamous-cell-carcinoma.
- Natalie Matthews, MD, MPhil, FAAD; Rajiv I. Nijhawan, MD, FACMS, FAAD; and Darrell S. Rigel, MD, FAAD, “Basal cell carcinoma: From symptoms to treatments,” American Academy of Dermatology Association, October 2025, https://www.aad.org/public/diseases/skin-cancer/basal-cell-carcinoma.
- Gaia Moretta, Tonia Samela, Francesca Sampogna, et al., “Attitudes among dermatologists regarding actinic keratosis treatment options,” Dermatology Reports, January 2022, https://pmc.ncbi.nlm.nih.gov/articles/PMC9577376/.

