Table of Contents
- Key Points
- What Is Hidradenitis Suppurativa?
- Hidradenitis Suppurativa Symptoms
- Hidradenitis Suppurativa Causes
- Hidradenitis Suppurativa Treatment Options
- Schedule Expert Hidradenitis Suppurativa Care Today
- References
Key Points
- Hidradenitis suppurativa (HS) is a chronic, commonly misunderstood inflammatory skin condition that impacts a large percentage of the population
- The symptoms, causes, and triggers of HS are wide-ranging and can deeply impact quality of life.
- Effective treatment exists and is highly personalized. From topical and oral antibiotics to FDA-approved biologics, surgical procedures, and lifestyle changes, there are many ways to manage HS.
A recent study on the global prevalence of hidradenitis suppurativa (HS) revealed some startling realities, enough to prompt urgent action from public health officials. For starters, the condition impacts a surprisingly large portion of the entire human population: upwards of 1 percent. Another revelation is that it takes an average of seven to ten years for patients to receive an accurate diagnosis.1
That staggering delay means years of pain, confusion, and unnecessary suffering for millions of people. If you have been living with recurring, painful lumps under your skin and have not yet found answers, you are not alone. More importantly, help is available. At Rogers Dermatology, we are committed to helping patients understand and manage complex skin conditions like HS with compassion and evidence-based care.
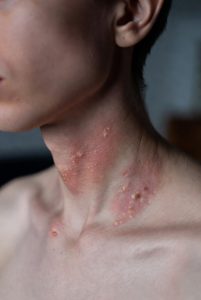
What Is Hidradenitis Suppurativa?
Hidradenitis suppurativa is a chronic, inflammatory skin condition that develops in areas where skin rubs together.2 Common areas include the:
- Armpits
- Groin
- Buttocks
- Inner thighs
- Under the breasts
The condition begins in the hair follicles, where blockages form and lead to the development of painful, deep nodules and abscesses. Over time, these lumps can rupture, drain, and leave behind significant scarring.
Common misconceptions about HS are that it is contagious, an infection, and is caused by poor hygiene. It is also frequently confused with cysts, boils, or folliculitis, which can lead to misdiagnosis and erroneous treatment protocols. HS is actually a systemic inflammatory disease closely linked to the immune system and has a strong genetic component.3
HS is classified into three stages of severity (known as the Hurley stages), ranging from “mild” (isolated nodules and no scarring) to severe (widespread abscesses, tunnels beneath the skin called sinus tracts, and extensive scarring). Early diagnosis and treatment are essential to slowing progression and protecting your quality of life.
Hidradenitis Suppurativa Symptoms
Hidradenitis suppurativa symptoms can range from mild discomfort to debilitating pain that significantly impacts daily life. Recognizing these signs early is crucial to getting timely care. The most common symptoms of HS include:
- Pea- to marble-sized lumps under the skin that may feel warm to the touch
- Recurring bumps that resemble boils or cysts, often appearing in skin folds
- Blackheads appearing in pairs or clusters (a hallmark sign of HS)
- Abscesses that rupture and drain foul-smelling pus
- Sinus tracts—tunnel-like channels beneath the skin connecting nodules
- Scarring and thickened skin in affected areas
- Persistent itching and burning sensations
- Flare-ups triggered by stress, hormonal changes, heat, or friction
It is important to note that HS is more than a condition impacting the skin. Many patients also experience significant psychological impacts, including depression and anxiety, due to chronic pain, scarring, and the social stigma often associated with the disease. If you are experiencing any of these symptoms, please do not wait to seek evaluation from a qualified dermatologist in Greenville.
Hidradenitis Suppurativa Causes
Understanding the underlying causes of hidradenitis suppurativa requires a look at multiple interconnected factors. Researchers have identified several key contributors:
- Follicular occlusion: HS begins when hair follicles become blocked, leading to rupture and an intense inflammatory response in the surrounding tissue.
- Immune system dysfunction: An overactive immune response plays a central role in HS, which is why many treatments target specific inflammatory pathways.
- Genetics: HS tends to run in families—up to 40 percent of patients report a family history of the condition, suggesting a strong hereditary component.4
- Hormonal influences: HS most commonly develops after puberty and disproportionately affects women, suggesting that hormones—particularly androgens — play a significant role.
- Obesity and metabolic factors: Excess weight can increase friction in skin folds and is associated with more severe disease, though HS affects individuals of all body types.5
- Smoking: Smoking is one of the strongest environmental risk factors for HS and has been linked to more frequent and severe flare-ups.
It is worth repeating: HS is not caused by a lack of cleanliness. Patients should never feel shame or embarrassment about their condition. It is a medical disease that deserves the same empathy and evidence-based care as any other chronic illness.
Hidradenitis Suppurativa Treatment Options
 Hidradenitis Suppurativa treatment is highly individualized, as the disease varies widely in severity and presentation from patient to patient. A comprehensive approach often combines lifestyle modifications, medical therapies, and in some cases, surgical intervention. Your dermatologist will work with you to build a treatment plan tailored to your specific stage of disease, symptoms, and goals.
Hidradenitis Suppurativa treatment is highly individualized, as the disease varies widely in severity and presentation from patient to patient. A comprehensive approach often combines lifestyle modifications, medical therapies, and in some cases, surgical intervention. Your dermatologist will work with you to build a treatment plan tailored to your specific stage of disease, symptoms, and goals.
Hidradenitis Suppurativa Medication
Hidradenitis Suppurativa medication options have expanded significantly in recent years, offering patients more hope than ever before. Common medical treatments include:
- Topical antibiotics (e.g., clindamycin): Effective for mild disease, applied directly to affected skin to reduce bacterial involvement and inflammation.
- Oral antibiotics (e.g., doxycycline, tetracycline combinations): Used for moderate disease and often prescribed for extended periods to manage flares and prevent new lesions.
- Biologics (e.g., Humira and Cosentyx): These work by targeting specific proteins in the inflammatory cascade and are typically reserved for moderate-to-severe cases of HS.
- Hormonal therapies: Oral contraceptives and anti-androgen medications can help reduce flares in some female patients.
- Retinoids: Oral retinoids like acitretin may be used in select cases to reduce follicular blockage.
- Corticosteroid injections: Used to rapidly reduce inflammation in individual, painful lesions.
- JAK inhibitors and newer targeted therapies: An exciting and growing area of research with promising results in clinical trials.6
Procedural and Surgical Treatment
For patients with more advanced or treatment-resistant disease, the following procedures may be recommended:
- Incision and drainage: A short-term measure for acutely painful abscesses, though it does not prevent recurrence.
- Laser therapy: Targets hair follicles in affected areas and can reduce flares and improve the appearance of scarring.
- Wide surgical excision: Removal of affected tissue in patients with severe, refractory disease. It carries a high success rate but requires a longer recovery period.
- Deroofing: Removing the top skin layer of painful abscess or sinus tunnels, to allow healing and reduce recurrence.7
Lifestyle Modifications
In addition to medical and procedural therapies, lifestyle changes can meaningfully reduce flares and improve overall well-being:
- Quitting smoking, which is one of the most impactful steps a patient can take
- Maintaining a healthy weight to reduce friction in skin folds
- Wearing loose-fitting, breathable clothing to minimize irritation
- Using gentle, fragrance-free cleansers in affected areas
- Managing stress through mindfulness, exercise, and adequate sleep
- Following an anti-inflammatory diet and identifying personal food triggers
Schedule Expert Hidradenitis Suppurativa Care Today
Living with hidradenitis suppurativa can feel isolating and overwhelming, but you do not have to navigate it alone. At Rogers Dermatology, our team has the expertise and compassion to help you achieve better control of your symptoms and quality of life. Whether you are newly diagnosed, have been managing HS for years, or are simply looking for a second opinion, we are here to help.
We stay current with the latest advances in hidradenitis suppurativa treatment and work collaboratively with each patient to find the most effective, personalized approach. If you are searching for a dermatologist Greenville patients trust for comprehensive, cutting-edge HS care, contact us today to schedule your appointment. Together, we can create a plan to help you take back control of your skin and your life.
References
-
- “First Global Prevalence Study into Hidradenitis Suppurativa reveals need for urgent action from policy makers GHiSA study confirms prevalence higher than previously thought,” International League of Dermatological Societies, December 2025, https://www.ilds.org/news-events/news/First-HS-GHiSA-Study/.
- Mayo Clinic Staff, “Hidradenitis suppurativa,” Mayo Clinic, March 2024,https://www.mayoclinic.org/diseases-conditions/hidradenitis-suppurativa/symptoms-causes/syc-20352306.
- “What is HS (Hidradenitis Suppurativa)?” HS Foundation, retrieved on February 23, 2026, from: https://www.hs-foundation.org/what-is-hs.
- Shannon M. Eble, Oliver J. Wisco, Luigi Boccuto, et al., “Genetic factors associated with hidradenitis suppurativa, a literature review,” International Journal of Women’s Dermatology, June 2024, https://pmc.ncbi.nlm.nih.gov/articles/PMC11177810/.
- Charles B. Kromann, Kristina S. Ibler, Viggo B. Kristiansen, and Gregor B.E. Jemec, “The influence of body weight on the prevalence and severity of hidradenitis suppurativa,” Acta Dermato-Venereologica, September 2014, https://pubmed.ncbi.nlm.nih.gov/24577555/.
- Paula Ludmann, MS, “Hidradenitis Suppurativa: Diagnosis and Treatment,” American Academy of Dermatology Association, March 2025, https://www.aad.org/public/diseases/a-z/hidradenitis-suppurativa-treatment.
- Ibid.

